[U26] Digital Health: emerging, versatile and scalable
A viable Health Ecosystem thrives with easy access to more services

Dear Reader,
This update in Product | Strategy | Innovation covers a key topic within a 3-Part Series on a Health Ecosystem with a broader scope than healthcare delivery. In the first Part, we provided an overview of a 3-Pillar model for the Health Ecosystem. This update provides more context on Digital Health before covering Improving Outcomes with Connected Care in the second Part of the Series. Digital Health is a very broad topic including prescription digital therapeutics, digital medicine, mobile medical apps extending capabilities of medical devices, companion apps with drugs, telemedicine and wellness apps for healthy living just for a start. Digital Health also provides the overall digital layer spanning not only the various technologies, but also the various ways to access care. This is another reason to cover Digital Health separately before diving into Connected Care.
We will cover Digital Health from two perspectives. One is based on how the Food and Drug Administration (FDA) recognizes Digital Health in the United States. The FDA is focused on medical applications, but also provides guidance on how companies can determine what regulatory authorities are relevant for a specific use case or application. The other perspective has a broader scope and categorizes Digital Health based on the level of evidence, risk and regulations involved. This perspective was proposed by a number of organizations who are championing Digital Health including the Digital Medicine Society, Digital Therapeutics Alliance, HealthXL and NODE.Health.
What’s in this topic for us? Digital Health can play a key role to advance Connected Care with multiple ways to access health-related services. Think of the Volkswagen Group with 3 core brands and products positioned with different capabilities and price points under Porsche, Audi and Volkswagen. You can buy or lease these vehicles. You can also use a ride-sharing service like Uber or Lyft to pay-by-the-mile to take a Volkswagen from point A to point B. Digital Health enables this “Uber option” when consumers can take some actions without a provider, but can also provide the Porsche or Audi when prescribed digital therapeutics or digital medicine are indicated and available through a provider. The Uber option is important for healthcare. We need to ensure no one is left behind and underserved populations can access care along with those with more disposable income or access to comprehensive health plans.
We will also consider the role Digital Health can play for Healthy Living and Prevention to augment Primary Care. Healthy Living and Prevention are two of the 9 points of innovation covered in our Health Ecosystem model under the Consumer Pillar. In this update, we will cover:
Overview of Digital Health,
Access to Digital Health, and
Role Digital Health can play in Healthy Living and Prevention.
After covering Digital Health in this update, we can then explore Connected Care with that background in the next Part of the Series.
1. Overview of Digital Health
Digital Health has evolved over the years as the fields of informatics, mobile computing, and telemedicine have advanced. Digital Health most likely originated during the early years of the telephone in the late 1800s with basic examples of “telehealth” to ask questions about symptoms or request medical assistance with an emergency. The Lancet documented an early case report on telemedicine in 1879 with a physician successfully diagnosing a child with a medical condition over the phone in the middle of the night.1 Wireless communication with radios further expanded telehealth and telemedicine into remote areas in the early 1900s.
The terms telehealth and telemedicine are often used interchangeably, but telehealth has a broader scope including non-clinical applications and the technology used to transmit voice, data and video. Telemedicine is focused on providing medical care to another location. Robotics can also enable telesurgery with a surgeon usually at a teaching hospital collaborating with a surgeon in a remote location to complete a surgical procedure without transporting the patient to the teaching hospital.
Telehealth is basically the Zoom web-conference equivalent for Digital Health. Not exactly the transformation we need to advance healthcare, but it does play a key role to expand access to care.
The first telemedicine clinic was established in 1967 at the Massachusetts General Hospital in Boston. NASA also developed technology around this time to monitor astronauts remotely as another telemedicine application in preparation for travel to space. Telemedicine has continued to evolve with 2-way video communication to remote areas. The Veterans Administration has increased its use of telemedicine to offer specialized care across multiple sites by a specialist based at a primary site.
Dr. Byron Brooks from the telemedicine program at the University of Texas Medical Branch in Galveston, TX co-founded Teladoc in Dallas, TX in 2002. Teladoc launched in 2005 as the first national telehealth provider. American Well (now Amwell) followed with another commercial telehealth platform. Early traction in Hawaii provided remote care when feasible across the islands to reduce the need to travel between islands to access similar care. A health system in Hawaii, its provider network, a health insurance provider and Amwell could partner to provide telemedicine services to the islands of Hawaii. Virtual Care is a model used by companies like Firefly Health to provide primary and limited specialty care virtually with their own contracted Provider Network using their own telemedicine platform to provide remote care to employers as a health benefit and individuals.
Telehealth is basically the Zoom web-conference equivalent for Digital Health. Not exactly the transformation we need to advance healthcare, but it does play a role to expand access to care. The FDA recognizes the following regulated areas of Digital Health through its Digital Health Center of Excellence.
Artificial Intelligence and Machine Learning (AI/ML) in Software as a Medical Device
Device Software Functions, including Mobile Medical Applications
The FDA also provides some guidance on mobile health apps using an online tool to determine what regulations potentially apply from the FDA, Federal Trade Commission (FTC) & Office of Civil Rights (OCR). Wellness apps, devices and media might exist outside of medical regulations, but are also subjected to an ever changing grey area of enforcement discretion by the FDA. An untended consequence is companies adopt a regulatory strategy to avoid medical regulations. Products should be positioned and developed with a strategy to address a market need. The regulatory strategy can then adapt to the product positioning.
A positive Digital Health trend includes medical device companies adding mobile medical applications to extend capabilities of cleared medical devices. This provides added value to patients who are prescribed these devices by a provider. Patients can download these apps from the Apple App Store and Google Play to their own mobile device. These apps are usually regulated by the FDA and other regulatory authorities outside the US. Examples include the Philips Respironics DreamMapper and ResMed myAir apps used by patients prescribed sleep therapy devices from these manufacturers. Both mobile medical apps help coach patients with some form of a sleep score for feedback on device use and adjustments that may be needed to optimize therapy.
Calm is consistently rated in the top ten for health and wellness apps and the #1 app on Apple’s App Store for sleep, meditation and relaxation.
Stand-alone wellness apps and/or instructional videos can provide value to individuals who are interested in access to solutions without a provider. Difficulty falling asleep might be due to difficulty unwinding at the end of busy days. Wellness apps Calm and Headspace were launched for relaxation, mindfulness and guided meditation. But consumer usage patterns indicated these apps were also being used to help users prepare for sleep. Calm is consistently rated in the top ten for health and wellness apps and the #1 app on Apple’s App Store for sleep, meditation and relaxation. Calm added Sleep Stories to help users fall asleep.

Fig. U26-1 illustrates Digital Health categorized based on different levels of evidence with varying degrees of risk and regulatory oversight. The broadest category of Digital Health includes non-clinical and clinical applications. Digital Medicine covers products and clinical research tools used to measure and/or intervene in the service of human health. The mobile medical apps mentioned above that extend the capabilities of a regulated medical device would typically fit into this Digital Medicine category. Wearable sensors for continuous glucose monitoring to detect low blood sugar with a mobile app extend the supervision of a provider so a patient can administer insulin as indicated would also typically fit into Digital Medicine.
Interventions might include products from a relatively new classification called Digital Therapeutics. This classification requires rigorously developed and design-controlled products with clear evidence to support claims of risk, efficacy and intended use. These products are regulated for medical use and typically require a prescription by a licensed provider. There are some applications where regulations permit use of a medical device without a prescription, but design control and product registration are still required. Digital Therapeutics are more likely to include a wearable sensor for closed-loop control of the intervention.
The current global market size for Digital Therapeutics is estimated at $4.2 billion for 2021 and is expected to grow 26% a year to reach $10.6 billion by 2025.2 HealthTech companies focused on Digital Health including Digital Therapeutics will scale with multiple solutions for different medical conditions. Pharmaceutical companies can also drive value for specific medical conditions with both pharmacotherapy and Digital Therapeutic solutions. Mental Health, Pain, Diabetes, Obesity and Neuroscience are some examples where pharmaceutical companies will likely integrate Digital Health. Novartis, Sanofi and Bayer are both active in the space.
2. Access to Digital Health
When access to care is limited through any of a number of factors, health outcomes are compromised. These factors can include the steps to schedule an appointment, time before the next available appointment with a provider and the cost to see a provider without a covered health plan. Consumers have access to Digital Health through retail locations, online and mobile apps. In many cases, Digital Health for consumers is available at minimal cost within minutes. This can also provide a hybrid where consumers investigate symptoms easily on a mobile app. If consumers are interested in pursuing a medical opinion or access medical treatment based on identification of symptoms and recommended next steps, the consumer could be connected to a provider to access medical care at a published fixed price.
Fig. U26-2 illustrates access to care for Consumers, through Employers and through Provider Networks (see columns in the illustration). Access is a balance between the requirements and burden to access care through a provider, but with the potential benefit of a definitive diagnosis and prescribed medical treatment. Access by going online as a consumer or using a wellness app downloaded immediately to an iPhone or Android smart phone may decrease the burden for access, but may only provide a more generalized solution. Cost may also vary where consumers pay out of pocket and care through a provider is likely covered by a health plan. Copays may reduce the cost benefit of health plans in cases where consumer solutions are comparable. And employers may provide additional benefits as part of health plans to offer the convenience of consumer solutions like wearable fitness trackers and/or gym membership for regular exercise and are covered compared to paying full price as a consumer.
Fig. U26-2 also shows the categorized solutions from Fig. U26-1 including Digital Health, Digital Medicine and Digital Therapeutics (see rows in the illustration). The Consumer column shows Digital Medicine* and Digital Therapeutics*. These are marked with an asterisk to indicate these would be available with limited use to consumers unless they connect to a provider to receive one of these solutions and then continue care as a consumer until there is a need to activate a provider again. This is not ideal. The better option is to stay under the care of a provider with access through the consumer pathway. This hybrid use case between Consumer and Provider Networks will need to evolve with commercial solutions from companies like Firefly Health, K Health, Walmart Health and CVS Minute Clinics. We will discuss that more under the second Part of the Series on Connected Care.
Rare diseases also fall into small markets where Digital Health solutions may have advantages to optimize for the requirements of the condition.
Where Digital Health can provide significant value is with platform solutions across all means of access on the bottom row of Fig. U26-2. That would also align with Healthy Living and Prevention in the Health Ecosystem model. We will cover these more in the section below. But a fitness tracker used at scale with consumers could also be leveraged by employers to improve performance of teams with additional coaching led by a certified trainer and provider networks could add both exercise physiologists and nutritionists to add fitness tracking to their primary care programs covered by participating health plans. Adherence is the key variable for sustained health outcomes, so a combination of health coaches and primary care providers encouraging adherence could be more effective than a purely digital solution.
Underserved populations typically include those with barriers to access care like the homeless, low-income, rural and migrant workers. But access to Digital Health also includes small markets that typically do not attract the attention of developers. Those underserved populations include and have been addressed by the solutions in parentheses: pediatric (prescribed digital therapeutic to improve vision in 4-7 yr olds diagnosed with amblyopia), elderly (VR therapy to relive experiences and explore new ones), pregnant (fetal monitor and companion app to track contractions) and other individuals who do not fall into the larger adult population.
Rare diseases also fall into small markets where Digital Health solutions may have advantages to optimize therapy for the condition. Spinal muscular atrophy (SMA) is a rare disease affecting about 1 in 11,000 live births and is a leading cause of genetic death in infants and a range of disabilities in teenagers and adults. Biogen has a drug approved for SMA and is investigating a companion app to track symptoms and monitor function with a wearable to improve outcomes.
Non-profit organizations can also help fund initial innovation into a specific disease, disorder or condition to advance Digital Health solutions with grants and awards. The Cystic Fibrosis Foundation (CFF) is a very active non-profit that has worked effectively with multiple stakeholders including the research community towards a cure. The CFF is sponsoring research to investigate the use of digital health companion apps with pharmacotherapy fr cystic fibrosis.
3. Role Digital Health can play in Healthy Living and Prevention
Wearable fitness trackers from companies like Whoop, FitBit, Apple, Samsung and Garmin have raised awareness around physical activity and the lack of exercise in our daily lives without scheduled programs that include walking, running, biking, hiking, swimming and other planned activities. These wearable sensors have also extended capabilities using the same hardware and additional software to estimate sleep time and depth of sleep. This is not sleep measured by monitoring brain activity, but uses body movement to estimate sleep. This can be relatively accurate in individuals without a sleep disorder that may lead to periods of “quiet” wakefulness when the brain is awake, but body movements do not correlate with this wakefulness.
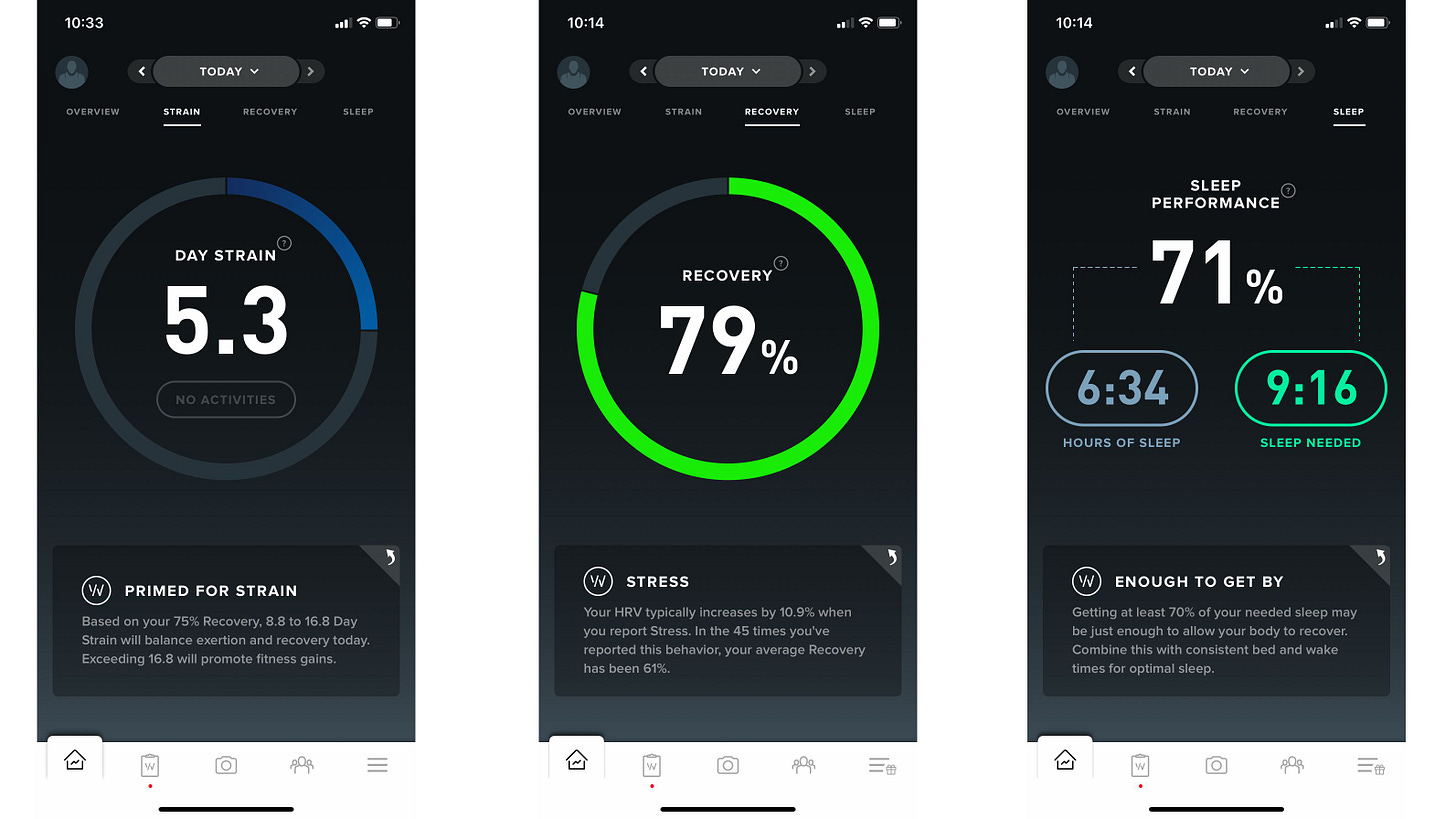
The WHOOP App provides a great proxy for user experience and how digital health can provide meaningful insights to coach and modify behavior to achieve better health outcomes.
The WHOOP App shown in Fig. U26-3 focuses on 3 key areas for healthy living using feedback on Sleep, Recovery and Strain. The WHOOP 4.0 wearable wrist band is less of a smart watch like the Apple Watch and more of a health and human performance wearable with the sensors needed to monitor movement, skin temperature, pulse rate and blood oxygen levels. WHOOP Sleep uses data collected to estimate the recommended hours of sleep for optimal recovery and monitors sleep for comparison to the recommended hours of sleep. WHOOP Recovery looks at heart rate variability, resting heart rate and sleep to provide feedback on your body’s readiness to perform on a scale of 0 to 100. WHOOP Strain measures your heart rate 24/7 to determine how much stress you are putting on your body using a scale of 0 to 21 with 18 to 21 indicating “over-reaching” with significant stress. WHOOP is leading the way with athletes, teams and individuals to improve human performance. The WHOOP App provides a great proxy for user experience and how digital health can provide meaningful insights to coach and modify behavior to achieve better health outcomes.
Philips provides healthy sleep solutions through its SmartSleep brand direct to consumers. These products complement and are in addition to regulated medical devices prescribed to patients through providers. The clinically validated Philips SmartSleep Analyzer is an online tool to help you determine in about 10 minutes what sleep issues might be keeping you up at night. But if you prefer to talk to a sleep physician, a Virtual Care Consult provided by Amwell is also available to make that connection on-demand. After completing the 10 minute questionnaire, the SmartSleep Analyzer provides insights on your sleep based on your responses. Philips also sells products & subscription services to address a number of these sleep issues with a SmartSleep Better Sleep Program, SmartSleep Deep Sleep Headband, SmartSleep Snoring Relief Band and SmartSleep Wake-Up Light.
Physical activity and sleep are two important factors for healthy living, but there are many more. The US Center for Disease Control (CDC) provides an overview of Healthy Living. Nutrition is an important factor to complement physical activity and sleep, but managing substance use and mental health are also important. Nutrition is an area in particular that is key to health living, yet negatively impacted by processed foods and a modern western diet. Sugar and carbohydrates in particular in processed foods have contributed to obesity and diabetes in more developed countries where disposable incomes enable eating out and buying prepared foods.
If it takes a village to raise a child, it takes an engaged local community to scale healthy living.
Monitoring food intake is more challenging than wearing a sensor to track physical activity. Documenting estimated calories and food types consumed during a meal can be done with logs, but the process should be easy. Future apps should only require a photo and machine learning to automate estimating calories and food type. Menus in restaurants and recipes should include a QR code to scan and input accurate info into apps on the food provided with a single serving.
Blue Apron and other meal-kit delivery companies developed the idea of a more streamlined way to prepare food at home 2 to 3 nights a week. This concept should evolve into a 7-day plan that includes both dining out or delivery with participating restaurants and meals prepared at home with participating local grocery stores or delivery services supplying the produce and ingredients. Apps and videos should guide the meal planning process, grocery lists, ordering groceries online for pick-up or delivery and recipes to prepare food at home. Recommendations for 7-day meal plans that include a specified number of meals eating out or delivery through participating restaurants also builds on the concept of a health ecosystem in a community. Corporate partners can incentivize healthy living using these plans when combined with physical activity that is also tracked to earn additional rewards. If it takes a village to raise a child, it takes an engaged community to scale healthy living.
Mental health is also a growing area of concern in our modern digital world, so advancing digital health requires addressing mental health, too. Meditation, relaxation, positive social interactions and cognitive skills are all feasible with digital tools and health & wellness apps. These apps have limitations without supervision by a healthcare provider, but are a starting point and can include access to a provider through virtual care or an in-person visit as needed. That could also result in using a different platform for care though a provider.
But as previously mentioned, just because the FDA does not regulate an area or product category today doesn’t mean they will not use enforcement discretion in the future.
Some daily routines are consistent with healthy living, but others are fundamental to prevention like oral health, heart health, pre-diabetes care and workplace ergonomics. Prevention according to FDA guidelines is regulated because the intended use and product claims will likely be tied to a medical condition versus health and well-being. But if the claims are around reducing risk factors that are not medical, then the use may fit a non-medical use case. But as previously mentioned, just because the FDA does not regulate an area or product category today doesn’t mean they will not use enforcement discretion in the future.
Omada Health was founded in 2011 as a digital health company with a mission to inspire and engage people in lifelong health one step at a time. The initial focus was on a digital diabetes prevention program (DPP) for individuals with pre-diabetes. Diet, weight management with a connected scale, physical exercise, sleep, mobile app, health coach and peer network are key components of the program. With over 450k members enrolled, the Omada digital DPP program is another proxy for digital health. Omada Health has also expanded with other programs including diabetes, musculoskeletal, hypertension and behavioral health. Omada Health uses the term digital care for the services provided to enable personalized care plans. As this model evolves over time, it will likely include all the categories we have discussed including digital health, digital medicine and digital therapeutics.
Conclusion
Healthcare faces many challenges that require more than just throwing technology at its problems, but Digital Health provides many opportunities to improve access to care and to improve outcomes with continuous and connected solutions. The hierarchy of Digital Health categories covered in Fig. U26-1 also combined with different ways to access care in Fig. U26-2 provides a digital layer to advance Connected Care. We will discuss Connected Care in the second Part of the 3-Part Series on a Health Ecosystem.
Just like the Volkswagen Group offers Porsche, Audi and Volkswagen to position vehicles with different capabilities and price points, Digital Health offers digital therapeutics (Porsche), digital medicine (Audi) and digital health (Volkswagen). Digital Health also provides a similar concept to Uber’s ride-sharing for consumers investigating symptoms using a chatbot or mobile app that can then connect to a licensed provider for a fixed price for a medical opinion. These providers are then provided machine learning ranked diagnosis options based on the query in-process that started with a consumer who has now opted in to become a patient for that encounter. K Health is innovating in this domain for urgent care, primary care, mental health and pediatrics with a mobile app and over 300 licensed providers to over 5 million people.
Digital Health enables consumers to cost-effectively do more to address Healthy Living and Prevention to achieve more positive health outcomes independent of or in collaboration with provider networks. Preventing pre-diabetes progressing to diabetes, improving heart health and using substances in moderation can be done with Digital Health to reduce risks that otherwise progress to poor health outcomes if left unmanaged. Bonds are used to build and expand the physical spaces for our hospitals and health systems to diagnose and treat our medical conditions. Communities should also consider bonds and other financial means to incentivize key areas for Healthy Living as discussed above and connect Consumers and Provider Networks with Digital Health to realize a viable community-based Health Ecosystem.
Best,
Stephen
I’m long GOOG and TDOC mentioned in this update. Nothing in this post is intended to serve as financial advice. Do your own research.
Bashshur R, Shannon GW (2009-01-01). History of Telemedicine: Evolution, Context, and Transformation. Mary Ann Liebert. ISBN 9781934854112.
The Business Research Company (2021-10-07). Digital Therapeutics Global Market Report 2021.